Tom Branna, Editorial Director11.21.18
Skin isn’t just the largest organ in the body, it’s one of the hardest working; performing myriad tasks such as regulating temperature, eliminating waste, and protecting the body from injury. The New York Society of Cosmetic Chemists’ symposium, Skin Barrier Disruption & Inflammation, was sponsored by Silab, Inc. Carine Mainzer, PhD, scientific support manager, Silab Inc., chaired the event and served as the first presenter, answering the question: "Upon barrier breakage and bacterial invasion, how do skin cells communicate to immune effectors?"
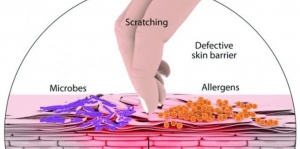
Mainzer reviewed the biology of skin, the skin barrier’s function and its disruption and the skin’s defenses. Some of the triggers for skin barrier problems include genetic factors, wounds, allergies, inflammation, seasonal humidity, age, fair pigmentation and even psychological stress.
"Indeed, the skin is a dynamic barrier that interacts and senses its environment," noted Mainzer. "Upon barrier breakage, the skin orchestrates a defense response that enables signaling the damage and the danger to surrounding cells including immune cells. One important aspect is the complex communication that takes place between epithelial/mesenchymal/immune cells through physical contact and through molecular mediators."
In a context mimicking some hallmarks of atopic dermatitis (barrier breakage and Staphylococcus aureus stress), this study underlined the important contribution of cutaneous cells in the immune barrier function, she explained.
"Through their active role in shaping the local inflammatory microenvironment, cutaneous cells have been demonstrated to activate key players in the initiation of the immune system, namely Langerhans cells and dendritic cells," noted Mainzer. "This data is of importance as a non-inflammatory microenvironment depicted only a maintenance effect on such cells."
According to the speaker, this study highlights a fine-tuning role of keratinocytes and fibroblasts secretions and their direct influence on neighboring cells in the skin, with a final impact on the immune barrier function. It also provides evidence that it may be possible to reinforce the barrier function by modulating or boosting such communication in the case of an adverse event as bacterial stress.
"This interconnected vision of the skin is an important aspect to keep in mind when developing topical skin care products and reveals that it is possible to maintain a strong barrier by stimulating cutaneous cells and their ability to shape the local microenvironment," she added.
The study is part of Silab’s collaboration with universities and research groups throughout the US. The goal of this collaboration is to develop scientific knowledge, new screening models and new actives, Mainzer concluded.
Mainzer benefitted from a post-doctoral fellowship sponsored by Silab at the University of California, San Francisco in the laboratory of Dr. Peter Elias MD. There, she conducted research on the exploration of intercellular communication and of note the power of the skin microenvironment in stimulating immune responses, with the eventual goal to improve skin barrier defenses. Mainzer was followed by Elias, who presented his research work on the "Topical therapy for atopic dermatitis: occlusive moisturizers vs. physiologic lipid barrier repair approaches."
“Every organism needs a barrier,” he noted. “It’s mostly about survival in a terrestrial environment, but that’s not all.”
Elias reviewed the protective functions of the stratum corneum, which include:
• Permeability barrier (allows life in a dry milieu);
• Exclusion of noxious chemicals and allergens;
• Protection from mechanical insults;
• Antimicrobial defense;
• Integrity and cohesion (desquamation);
• Antioxidant defense;
• Cytokine activation (outpost of immune system);
• UVB absorption;
• Hydration; and
• Neurosensory interface.
After that, he gave a brief overview of the classic stratum corneum model; i.e., corneocytes (bricks), extracellular matrix (mortar) and non-polar lamellar bilayers, which include cholesterol, long-chain fatty acids and ceramides. But bricks and mortar aren’t enough to build a competent permeability barrier, noted Elias.
“Skin needs the correct three lipids, which are cholesterol, free fatty acids and ceramides in the correct proportion (1:1:1 molar ratio) in a sufficient amount,” he explained.
That sufficient amount should be 10% of the weight of the stratum corneum and it should be organized correctly. Why should we care so much about the health and viability of this barrier?
Why Should We Care?
Skin maladies such as atopic dermatitis and psoriasis are on the rise and are caused by barrier abnormalities which can impact vulnerable populations, including young and old (from neonatal skin to aged skin) and even stressed skin, Elias pointed out.
“Topical therapies can aggravate, rather than help,” he added.
The speaker pointed out that there has been an epidemic of atopic disease in the past 50 years. The acquired insults that trigger atopic dermatitis against a genetically-vulnerable background include: secondary colonization with S. aureus, high pH soaps and surfactants, prolonged exposure to low humidity, insufficient exposure to UVB, increased psychological stress and air pollution. Elias also explained how high skin pH results in a filaggrin deficiency which leads to atopic dermatitis.
Corrective barrier repair therapy calls for a physiologic lipid-based formula that includes ceramides, free fatty acids and cholesterol, which are incorporated into lamellar layers.
The Right Ratio
“But the barrier is only repaired if the ingredients are in the correct molar ratio,” he reminded attendees. “Ceramides alone make the barrier worse!”
All three lipids, cholesterol, free fatty acids and ceramides, are required for barrier recovery. Normal barrier recovery occurs with an equimolar ratio of the “Big Three,” but accelerated recovery occurs after topical application of an “optical molar (3:1:1) ratio of the Big Three,” according to Elias.
How do these ingredients boost an anti-inflammatory response in atopic dermatitis? By normalizing the barrier, preventing allergen/hapten ingress, increasing the skin’s antimicrobial defense and normalizing pH.
“Some free fatty acids are anti-inflammatory,” he added.
Elias concluded by urging researchers to assess products in “sensitive skin” subjects. At the same time, he suggested that subjects should be assessed for any underlying skin problems and when they use a topical treatment, they should apply a small amount of the formula to assess any reaction. Finally, Elias said researchers should consider monitoring with an objective measure to track benefits and possible toxicity of the formulas.
The symposium was the last technical meeting of the NYSCC ahead of the Society of Cosmetic Chemists’ annual meeting (December 11 and 12) in New York City. But the chapter isn’t taking the rest of the year off; the annual NYSCC Supports Education Night will take place on Tuesday night at Stage 48 in Hell’s Kitchen. Proceeds from the event go to several universities and research programs that furthers the mission of the NYSCC. Stage 48 is a four-level, converted industrial space that incorporates New York’s old west side feel with modern amenities and state of the art sound and lighting. The venue features a grand ballroom with an extravagant mezzanine, a private lounge level with a performance space and a rooftop terrace with a gorgeous view of the Manhattan skyline. For tickets, visit www.nyscc.org. Questions? Contact Giorgino Macalino, awards@nyscc.org
Mainzer reviewed the biology of skin, the skin barrier’s function and its disruption and the skin’s defenses. Some of the triggers for skin barrier problems include genetic factors, wounds, allergies, inflammation, seasonal humidity, age, fair pigmentation and even psychological stress.
"Indeed, the skin is a dynamic barrier that interacts and senses its environment," noted Mainzer. "Upon barrier breakage, the skin orchestrates a defense response that enables signaling the damage and the danger to surrounding cells including immune cells. One important aspect is the complex communication that takes place between epithelial/mesenchymal/immune cells through physical contact and through molecular mediators."
In a context mimicking some hallmarks of atopic dermatitis (barrier breakage and Staphylococcus aureus stress), this study underlined the important contribution of cutaneous cells in the immune barrier function, she explained.
"Through their active role in shaping the local inflammatory microenvironment, cutaneous cells have been demonstrated to activate key players in the initiation of the immune system, namely Langerhans cells and dendritic cells," noted Mainzer. "This data is of importance as a non-inflammatory microenvironment depicted only a maintenance effect on such cells."
According to the speaker, this study highlights a fine-tuning role of keratinocytes and fibroblasts secretions and their direct influence on neighboring cells in the skin, with a final impact on the immune barrier function. It also provides evidence that it may be possible to reinforce the barrier function by modulating or boosting such communication in the case of an adverse event as bacterial stress.
"This interconnected vision of the skin is an important aspect to keep in mind when developing topical skin care products and reveals that it is possible to maintain a strong barrier by stimulating cutaneous cells and their ability to shape the local microenvironment," she added.
The study is part of Silab’s collaboration with universities and research groups throughout the US. The goal of this collaboration is to develop scientific knowledge, new screening models and new actives, Mainzer concluded.
Mainzer benefitted from a post-doctoral fellowship sponsored by Silab at the University of California, San Francisco in the laboratory of Dr. Peter Elias MD. There, she conducted research on the exploration of intercellular communication and of note the power of the skin microenvironment in stimulating immune responses, with the eventual goal to improve skin barrier defenses. Mainzer was followed by Elias, who presented his research work on the "Topical therapy for atopic dermatitis: occlusive moisturizers vs. physiologic lipid barrier repair approaches."
“Every organism needs a barrier,” he noted. “It’s mostly about survival in a terrestrial environment, but that’s not all.”
Elias reviewed the protective functions of the stratum corneum, which include:
• Permeability barrier (allows life in a dry milieu);
• Exclusion of noxious chemicals and allergens;
• Protection from mechanical insults;
• Antimicrobial defense;
• Integrity and cohesion (desquamation);
• Antioxidant defense;
• Cytokine activation (outpost of immune system);
• UVB absorption;
• Hydration; and
• Neurosensory interface.
After that, he gave a brief overview of the classic stratum corneum model; i.e., corneocytes (bricks), extracellular matrix (mortar) and non-polar lamellar bilayers, which include cholesterol, long-chain fatty acids and ceramides. But bricks and mortar aren’t enough to build a competent permeability barrier, noted Elias.
“Skin needs the correct three lipids, which are cholesterol, free fatty acids and ceramides in the correct proportion (1:1:1 molar ratio) in a sufficient amount,” he explained.
That sufficient amount should be 10% of the weight of the stratum corneum and it should be organized correctly. Why should we care so much about the health and viability of this barrier?
Why Should We Care?
Skin maladies such as atopic dermatitis and psoriasis are on the rise and are caused by barrier abnormalities which can impact vulnerable populations, including young and old (from neonatal skin to aged skin) and even stressed skin, Elias pointed out.
“Topical therapies can aggravate, rather than help,” he added.
The speaker pointed out that there has been an epidemic of atopic disease in the past 50 years. The acquired insults that trigger atopic dermatitis against a genetically-vulnerable background include: secondary colonization with S. aureus, high pH soaps and surfactants, prolonged exposure to low humidity, insufficient exposure to UVB, increased psychological stress and air pollution. Elias also explained how high skin pH results in a filaggrin deficiency which leads to atopic dermatitis.
Corrective barrier repair therapy calls for a physiologic lipid-based formula that includes ceramides, free fatty acids and cholesterol, which are incorporated into lamellar layers.
The Right Ratio
“But the barrier is only repaired if the ingredients are in the correct molar ratio,” he reminded attendees. “Ceramides alone make the barrier worse!”
All three lipids, cholesterol, free fatty acids and ceramides, are required for barrier recovery. Normal barrier recovery occurs with an equimolar ratio of the “Big Three,” but accelerated recovery occurs after topical application of an “optical molar (3:1:1) ratio of the Big Three,” according to Elias.
How do these ingredients boost an anti-inflammatory response in atopic dermatitis? By normalizing the barrier, preventing allergen/hapten ingress, increasing the skin’s antimicrobial defense and normalizing pH.
“Some free fatty acids are anti-inflammatory,” he added.
Elias concluded by urging researchers to assess products in “sensitive skin” subjects. At the same time, he suggested that subjects should be assessed for any underlying skin problems and when they use a topical treatment, they should apply a small amount of the formula to assess any reaction. Finally, Elias said researchers should consider monitoring with an objective measure to track benefits and possible toxicity of the formulas.
The symposium was the last technical meeting of the NYSCC ahead of the Society of Cosmetic Chemists’ annual meeting (December 11 and 12) in New York City. But the chapter isn’t taking the rest of the year off; the annual NYSCC Supports Education Night will take place on Tuesday night at Stage 48 in Hell’s Kitchen. Proceeds from the event go to several universities and research programs that furthers the mission of the NYSCC. Stage 48 is a four-level, converted industrial space that incorporates New York’s old west side feel with modern amenities and state of the art sound and lighting. The venue features a grand ballroom with an extravagant mezzanine, a private lounge level with a performance space and a rooftop terrace with a gorgeous view of the Manhattan skyline. For tickets, visit www.nyscc.org. Questions? Contact Giorgino Macalino, awards@nyscc.org