Nava Dayan, Dr. Nava Dayan LLC05.02.16
The outer layer of the cornea is composed of epithelial tissue, which acts as a barrier to protect the cornea and the eye. The corneal epithelium consists of several layers of cells including a surface epithelium, a central, thicker stroma, and an inner endothelium. Although there are no blood vessels in the cornea it is innervated. Damage to the eye can be of greater impact to quality of life when compared to scars on the skin since it may affect vision. Penetrating insult to an organ typically generates a fibrotic tissue to quickly repair it. This fibrotic tissue is malfunctioning. In the cornea, fibrotic repair presents special challenges and may affect both clarity and shape of the cornea.
Perhaps the most common alerting safety concern related to eye care products (for skin treatments intended for the eye area as well as color cosmetics) is microbial contamination and this is also a reason for recalls of marketed products. Although this is definitely an issue of concern that deserves attention, this column will not address testing of proper preservation. It will focus on testing for eye irritation, a chemical, non-bacteria-related reaction, when a compound or combination of compounds can cause such reactions to the eye.
In 2012, a study by Cardiff University in the UK pointed out that the use of multiple eye cosmetics is extensive in Western populations and associated with the perception of ocular discomfort. Scientists advised that since such products are widely used on a daily basis, more research is required to assess the effect on the ocular surface and tear film as those effects may be underestimated. A later publication from 2015 by the School of Optometry and Vision Science in Canada outlines that color cosmetics may accumulate within the eye lacrimal system and conjunctivae over many years of use, but immediate reports of eye discomfort after application are most common.
The researchers further point out that creams used around the eyes may have negative effects on the meibomian gland function and may be a contributing factor to dry eye disease. The meibomian gland is a lipid-secreting gland of the eye; its secretions mix with tears to lubricate the eye similar to sebaceous gland on skin.
Three Test Methods
This column will focus on describing three methods for assessment of eye irritation: the Bovine Cornea Opacity and Permeability Test (BCOP), the Chorioallantoic Membrane Vascular Assay (CAMVA) and the Epiocular model assay, each has specific advantages and limitations, some will be described here. If the formulation’s or ingredient-of-interest’s intended use is around the eye area and/or if specific results are inconclusive, it is highly recommended to run all three studies. If the tested formulation or ingredient already demonstrated skin irritation, the affected concentration should be considered in the eye irritation study design.
Since the cornea is of primary interest in assessing ocular irritation, the BCOP provides a useful parallel for possible human exposure. BCOP utilizes bovine cornea obtained from slaughterhouses. Although the tissue is obtained from an animal, in some cases, it is not considered an animal study; therefore, it is used for testing cosmetic ingredients. The company that develops and sells the tested article may determine if this assay is acceptable in accordance to its internal policy, ideology, values and compliance with market geographic location regulations.
BCOP Classifications
The BCOP classifies tested compounds on a scale of none, mild, moderate or severe irritants. It is based on the observation that a corrosive compound, such as a strong base, may cause denaturation and coagulation of corneal proteins thereby leading to irreversible opacity. This assay requires that a freshly obtained cornea is clamped between two chambers filled with physiologic saline solution followed by measuring the transmittance of light through the cornea. Since irritants are expected to generate cornea opacity, there is an inverse correlation between light transmittance and irritation when determined by an opacitometer, an instrument that measures light penetration through the cornea. The compound can be tested at any concentration and over a range of exposure times to differentiate between potential mild to severe eye irritants.
By this method, the higher the irritation the lower the transmittance due to increased opacity. In addition to light diffusion, at a later stage in the protocol development, a measurement of corneal permeability has been included. Here sodium fluorescein solution is added to the epithelial side of the chamber and the permeability of the fluorescent compound is quantified by measuring absorbance at 490nm. A clear advantage of this test is the use of relevant tissue for the endpoint since it uses a fresh intact cornea. In addition, as mentioned, it is not considered an in vivo animal test, is relatively inexpensive and quantitative. The test should be conducted by a highly skilled lab technician since inadequate clamping of the cornea to the chamber may cause indentation to its edges and edema—physical changes that may affect the validity of study results. Still, this assay presents some limitations. The solution that fills the chamber, although it maintains its viability for the duration of the assay, is not identical to the natural medium of the eye and is remote from in vivo conditions; i.e., it is static and not renewing.
In addition, criticism has been expressed to the fact that the assay cannot clearly differentiate between opacity cased due to irritation or such that is triggered by edema. Although both types of damages are relevant to risk assessment determination, in vivo the recovery from these conditions can be different.
CAMVA
The chorioallantoic membrane vascular assay (CAMVA) is an alternative to the Draize rabbit eye irritation method. In this assay, a vascularized membrane of a fertile hen’s egg is used to assess potential for eye irritation. It follows the magnitude of changes in the membrane upon exposure to a tested compound. The assessed damage to the vascular structure can be on hemorrhage, capillary injection or other.
In this assay, fertile white DeKalb XL or White Leghorn eggs are used. The eggs are incubated for 14 days during which their trays are rotated. On the fourth day of the incubation, the position of the embryo is determined and a small hole is drilled into the narrow end of the egg to allow the removal of the albumen after which it is sealed and a rectangular window is cut through the egg shell, the opening is covered and the egg is returned to the incubator. On Day 14 of the incubation, the eggs are removed and the tape is peeled to allow the examination of the chorioallantoic membrane.
The first stage of the study is screening a range of concentrations to determine potential effect. It is recommended that the selected concentrations are based on prior knowledge to refrain from the need to repeat the screening test in case no threshold of damage can be determined. The second stage of the study involves exposure of broader concentration range in an attempt to obtain dose response curve.
The assay uses distilled water or corn oil as preferred vehicles depending on the solubility of the tested compound. Both liquids and solids can be tested in this method, which is considered relatively rapid and cost-effective. In this assay, 30 minutes after dosing with the compound of interest, the eggs are removed from the incubator and the membrane is exposed and observed for abnormalities. A value of RC50 which is the calculated concentration theoretically producing a reaction in 50% of the treated eggs is determined. The assay allows classification into a non-irritant, indeterminate and irritant.
EpiOcular Eye Irritation Test
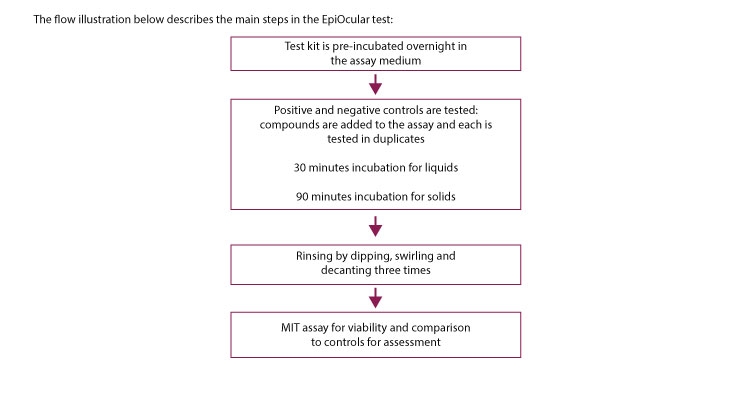
The two methods described, BCOP and CAMVA, use animal parts; therefore, they encounter the limitation of being biologically distanced from that of human exposure since the cells in those systems are animal cells. The EpiOcular Eye Irritation Test (EIT) utilizes human cells. The EIT was implemented in 2015 into the OECD Test Guidelines as TG 492. This three-dimensional reconstructed tissue is designed to mimic human cornea which is different from human skin in that it is non-keratinized/non-cornified and therefore, is more permeable when compared to a skin tissue model.
This in vitro test is aimed at hazard identification of compounds using a human derived cornea-like model. Specifically, it utilizes a three-dimensional reconstructed human cornea-like epithelial (RhCE) tissue model that is based on normal human cells. The EIT allows for differentiating between ocular irritants and corrosives. The test utilizes two separate protocols, one designed for liquid chemicals and a second, slightly modified protocol for solid test articles. The EIT prediction model uses a single exposure period (30 minutes for liquids, 6 hours for solids) and single tissue viability limits. The limit is 60% as determined by viability obtained by MTT assay. For detailed explanation on MTT, see my previous column on cell cytotoxicity (September, 2015).
In summary, facial skin care products, and especially those that are intended to apply to the skin around the eye, the lids or lashes, may come in contact with the eye. The eye is an organ that is different from skin in its permeability, biology and overall function. Therefore, eye irritation should be tested using specialized protocols.
Three such protocols are described in this column and additional protocals are available if further customization is required.
References:
Fini ME and, Stramer BM. Cornea. 2005 Nov;24(8 Suppl):S2-S11.
Ng A et al, Ophthalmic Physiol Opt. 2012 Nov;32(6):501-7.
Ng A et al, Eye Contact Lens. 2015 Sep 21
Bagley D.M. et al Toxicol In Vitro. 1999 Apr;13(2):285-93.
Kaluzhny Y. et al J Vis Exp. 2015 Aug 23;(102). doi: 10.3791/52979.
Nava Dayan
Owner
Dr. Nava Dayan LLC
Nava Dayan Ph.D. is the owner of Dr. Nava Dayan L.L.C, a skin science and research consultancy and serving the pharmaceutical, cosmetic, and personal care industries. She has 25 years of experience in the skin care segment, and more than 150 publication credits.
Tel: 201-206-7341
E-mail: nava.dayan@verizon.net
Perhaps the most common alerting safety concern related to eye care products (for skin treatments intended for the eye area as well as color cosmetics) is microbial contamination and this is also a reason for recalls of marketed products. Although this is definitely an issue of concern that deserves attention, this column will not address testing of proper preservation. It will focus on testing for eye irritation, a chemical, non-bacteria-related reaction, when a compound or combination of compounds can cause such reactions to the eye.
In 2012, a study by Cardiff University in the UK pointed out that the use of multiple eye cosmetics is extensive in Western populations and associated with the perception of ocular discomfort. Scientists advised that since such products are widely used on a daily basis, more research is required to assess the effect on the ocular surface and tear film as those effects may be underestimated. A later publication from 2015 by the School of Optometry and Vision Science in Canada outlines that color cosmetics may accumulate within the eye lacrimal system and conjunctivae over many years of use, but immediate reports of eye discomfort after application are most common.
The researchers further point out that creams used around the eyes may have negative effects on the meibomian gland function and may be a contributing factor to dry eye disease. The meibomian gland is a lipid-secreting gland of the eye; its secretions mix with tears to lubricate the eye similar to sebaceous gland on skin.
Three Test Methods
This column will focus on describing three methods for assessment of eye irritation: the Bovine Cornea Opacity and Permeability Test (BCOP), the Chorioallantoic Membrane Vascular Assay (CAMVA) and the Epiocular model assay, each has specific advantages and limitations, some will be described here. If the formulation’s or ingredient-of-interest’s intended use is around the eye area and/or if specific results are inconclusive, it is highly recommended to run all three studies. If the tested formulation or ingredient already demonstrated skin irritation, the affected concentration should be considered in the eye irritation study design.
Since the cornea is of primary interest in assessing ocular irritation, the BCOP provides a useful parallel for possible human exposure. BCOP utilizes bovine cornea obtained from slaughterhouses. Although the tissue is obtained from an animal, in some cases, it is not considered an animal study; therefore, it is used for testing cosmetic ingredients. The company that develops and sells the tested article may determine if this assay is acceptable in accordance to its internal policy, ideology, values and compliance with market geographic location regulations.
BCOP Classifications
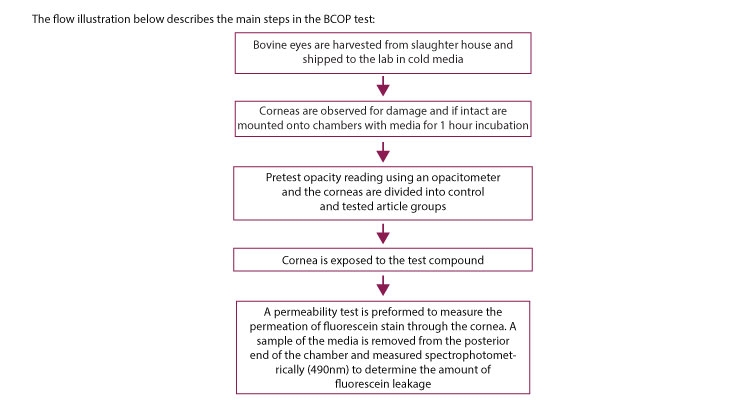
The BCOP classifies tested compounds on a scale of none, mild, moderate or severe irritants. It is based on the observation that a corrosive compound, such as a strong base, may cause denaturation and coagulation of corneal proteins thereby leading to irreversible opacity. This assay requires that a freshly obtained cornea is clamped between two chambers filled with physiologic saline solution followed by measuring the transmittance of light through the cornea. Since irritants are expected to generate cornea opacity, there is an inverse correlation between light transmittance and irritation when determined by an opacitometer, an instrument that measures light penetration through the cornea. The compound can be tested at any concentration and over a range of exposure times to differentiate between potential mild to severe eye irritants.
By this method, the higher the irritation the lower the transmittance due to increased opacity. In addition to light diffusion, at a later stage in the protocol development, a measurement of corneal permeability has been included. Here sodium fluorescein solution is added to the epithelial side of the chamber and the permeability of the fluorescent compound is quantified by measuring absorbance at 490nm. A clear advantage of this test is the use of relevant tissue for the endpoint since it uses a fresh intact cornea. In addition, as mentioned, it is not considered an in vivo animal test, is relatively inexpensive and quantitative. The test should be conducted by a highly skilled lab technician since inadequate clamping of the cornea to the chamber may cause indentation to its edges and edema—physical changes that may affect the validity of study results. Still, this assay presents some limitations. The solution that fills the chamber, although it maintains its viability for the duration of the assay, is not identical to the natural medium of the eye and is remote from in vivo conditions; i.e., it is static and not renewing.
In addition, criticism has been expressed to the fact that the assay cannot clearly differentiate between opacity cased due to irritation or such that is triggered by edema. Although both types of damages are relevant to risk assessment determination, in vivo the recovery from these conditions can be different.
CAMVA
The chorioallantoic membrane vascular assay (CAMVA) is an alternative to the Draize rabbit eye irritation method. In this assay, a vascularized membrane of a fertile hen’s egg is used to assess potential for eye irritation. It follows the magnitude of changes in the membrane upon exposure to a tested compound. The assessed damage to the vascular structure can be on hemorrhage, capillary injection or other.
In this assay, fertile white DeKalb XL or White Leghorn eggs are used. The eggs are incubated for 14 days during which their trays are rotated. On the fourth day of the incubation, the position of the embryo is determined and a small hole is drilled into the narrow end of the egg to allow the removal of the albumen after which it is sealed and a rectangular window is cut through the egg shell, the opening is covered and the egg is returned to the incubator. On Day 14 of the incubation, the eggs are removed and the tape is peeled to allow the examination of the chorioallantoic membrane.
The first stage of the study is screening a range of concentrations to determine potential effect. It is recommended that the selected concentrations are based on prior knowledge to refrain from the need to repeat the screening test in case no threshold of damage can be determined. The second stage of the study involves exposure of broader concentration range in an attempt to obtain dose response curve.
The assay uses distilled water or corn oil as preferred vehicles depending on the solubility of the tested compound. Both liquids and solids can be tested in this method, which is considered relatively rapid and cost-effective. In this assay, 30 minutes after dosing with the compound of interest, the eggs are removed from the incubator and the membrane is exposed and observed for abnormalities. A value of RC50 which is the calculated concentration theoretically producing a reaction in 50% of the treated eggs is determined. The assay allows classification into a non-irritant, indeterminate and irritant.
EpiOcular Eye Irritation Test
The two methods described, BCOP and CAMVA, use animal parts; therefore, they encounter the limitation of being biologically distanced from that of human exposure since the cells in those systems are animal cells. The EpiOcular Eye Irritation Test (EIT) utilizes human cells. The EIT was implemented in 2015 into the OECD Test Guidelines as TG 492. This three-dimensional reconstructed tissue is designed to mimic human cornea which is different from human skin in that it is non-keratinized/non-cornified and therefore, is more permeable when compared to a skin tissue model.
This in vitro test is aimed at hazard identification of compounds using a human derived cornea-like model. Specifically, it utilizes a three-dimensional reconstructed human cornea-like epithelial (RhCE) tissue model that is based on normal human cells. The EIT allows for differentiating between ocular irritants and corrosives. The test utilizes two separate protocols, one designed for liquid chemicals and a second, slightly modified protocol for solid test articles. The EIT prediction model uses a single exposure period (30 minutes for liquids, 6 hours for solids) and single tissue viability limits. The limit is 60% as determined by viability obtained by MTT assay. For detailed explanation on MTT, see my previous column on cell cytotoxicity (September, 2015).
In summary, facial skin care products, and especially those that are intended to apply to the skin around the eye, the lids or lashes, may come in contact with the eye. The eye is an organ that is different from skin in its permeability, biology and overall function. Therefore, eye irritation should be tested using specialized protocols.
Three such protocols are described in this column and additional protocals are available if further customization is required.
References:
Fini ME and, Stramer BM. Cornea. 2005 Nov;24(8 Suppl):S2-S11.
Ng A et al, Ophthalmic Physiol Opt. 2012 Nov;32(6):501-7.
Ng A et al, Eye Contact Lens. 2015 Sep 21
Bagley D.M. et al Toxicol In Vitro. 1999 Apr;13(2):285-93.
Kaluzhny Y. et al J Vis Exp. 2015 Aug 23;(102). doi: 10.3791/52979.
Nava Dayan
Owner
Dr. Nava Dayan LLC
Nava Dayan Ph.D. is the owner of Dr. Nava Dayan L.L.C, a skin science and research consultancy and serving the pharmaceutical, cosmetic, and personal care industries. She has 25 years of experience in the skin care segment, and more than 150 publication credits.
Tel: 201-206-7341
E-mail: nava.dayan@verizon.net